February 18, 2022
Investing in Culturally Sensitive Medical Care: How Mission-Based Financing Fills a Gap
Community development financial institutions helped develop financing solutions for healthcare facilities in rural America.

When the Coquille Indian Tribe in southwestern Oregon outgrew its 20-year-old medical clinic, the tribe dreamed of creating a larger initiative to help improve residents’ health through holistic wellness services.
That vision became a reality through innovative investment strategies provided by community development financial institutions (CDFIs). These mission-driven financial organizations are designed to invest in community initiatives that traditional institutions like banks might find too risky.
The result has been culturally sensitive, community-led healthcare initiatives that are helping shore up rural medical services even as the pandemic is shaking rural America’s already fragile healthcare delivery system.
A Home for Healing
The Ko-Kwel Wellness Center is housed in an 8,000-square-foot building located on the Kilkich Reservation of the Coquille Indian Tribe. The facility is Oregon’s first tribal center that offers services to the general public in addition to tribal members.
When tribal developers shared their vision with community development financial institution (CDFI) Craft3, the regional lender stepped forward with a New Markets Tax Credit allocation to secure the necessary equity. New Markets Tax Credits are designed to help attract private funders to high-impact projects in historically underserved communities. The unique financing package for the Ko-Kwel Wellness Center also includes several private grants and two long-term, affordable loans, one from Craft3 and another from a Maine-based CDFI, Coastal Enterprises, Inc. (CEI), both via the USDA’s Community Facilities program.
Potlatch, or sharing with one’s neighbors, is a core value of the Coquille people. Offering primary and dental care, behavioral health, a pharmacy, and other services, the center is “an exciting opportunity to apply our potlatch tradition of community sharing,” said tribal Chairman Brenda Meade. “It will be another option for people who have had trouble finding a healthcare provider.”
The center will make medical, dental and pharmacy services accessible to thousands of low-income families, and it will treat American Indian/Alaska Native patients at zero out-of-pocket cost. The center also has dedicated community gathering space and the facility will display Coquille artwork and craftmanship, in part to demonstrate tribal values.
The tribe intentionally named Ko-Kwel a “wellness center” to reflect a focus on serving each patient’s overall needs. The center emphasizes trauma-informed care and the comfort of cultural connection, addressing the unique needs of its core patient population and smoothing barriers to access.
“We want to care for the whole person,” Meade explained. “People will be able to get primary medical care, dental care and a pharmacy, all under one roof. And we don’t want to stop there. Over time, we want to add alternative therapies, such as massage, acupuncture and chiropractic. Our goal is to be able to take care of the whole person, not just the part that needs a prescription. We’re creating a holistic wellness experience, in keeping with our people’s traditional values.”
The late and much-loved Coquille Indian Tribe Chief Don Ivy went one step further: “This is a home for healing.”
Why Healthcare Centers Struggle to Access Financing
To operate, nonprofit healthcare centers typically rely on a combination of government grants, philanthropic support, donations, and payments from individuals, insurance companies, and government programs like Medicaid and Medicare. But as centers launch and grow to meet community needs, startup and expansion costs can often exceed fundraising and fee income, making it necessary for healthcare centers to seek financing for construction, operating capital, and/or equipment purchases.
The challenge for traditional financers is that balance sheets and financial projections for healthcare centers don’t resemble those of a typical business. It takes time for healthcare centers to secure payments for service from individuals and reimbursements from government entities. Furthermore, “receivables” are tough to value and lend against in comparison to real estate or other tangible hard assets. As underwriters who also borrow capital from public and private sources, CDFIs can be more flexible, particularly when mission alignment is factored into loan-to-value calculations.

Island Health and Wellbeing
Residents of Lāna‘i, Hawai‘i’s smallest inhabited island, are largely Filipino and Native Hawaiian, and 10.3% of households face some level of linguistic isolation. They face physical isolation too: it’s a $200 plus roundtrip flight from Honolulu or a $60 ferry ride from Lāna‘i to Maui. For the 44% of the island’s population that live at or below 200% of the Federal poverty level, the only option for affordable on-island health care is the Lāna‘i Community Health Center (LCHC).
Founded by two women, public health nurse and Native Hawaiian Jackie Woosley and educator Phyllis McOmber, in 2007, Lāna‘i Community Health Center was created to provide healthcare services in a culturally sensitive manner in accordance with their motto: E Ola Nō Lāna’i – Life, Health and Well-Being for Lāna‘i. The clinic staff is largely locals and caregivers reflecting the populations they serve. Written and oral translation is readily available. It emphasizes community values – for example, information on Covid-19 prevention focused on protecting the community’s Kūpuna, or elders.
Prior to 2015, Lāna‘i Community Health Center operated from a converted three-bedroom home on a steep hill. A lack of space limited services, even though the Center was the primary care provider for the island’s year-round population. Leadership had a vision for a new building with diagnostic technology like mammography, dental care, and other services considered standard in high-income and urban places.
But the health care provider struggled to put together a financial package to pay for it. Grants and scant private financing were not enough. The project required a government subsidy to lessen the developer’s dependence on private capital. That led to a creative solution proposed by CEI Capital Management, CEI’s New Markets Tax Credit subsidiary. The Lāna‘i project was a perfect match for CEI, whose mission focuses on growing good jobs, environmentally sustainable enterprises, and shared prosperity in rural regions throughout the U.S.
The new health center is in the center of Lāna‘i City, where 95% of the island’s population resides. In addition to being more accessible by foot, the new space expanded medical service offerings, including dental, and includes a community room, for free wellness programming. Throughout the pandemic, LCHC has served as a resource for Covid-19 testing, vaccinations, and food distribution.
Their community-centric approach is working. A fitness challenge held by LCHC in October 2020 had over 800 registrants, accounting for over a quarter of the island’s population. The participants in a hypertension monitoring program increased by six percent year over year, and participation in chronic disease programs also increases yearly. Lāna‘i Community Health Center has used their status as a community hub to increase access and reduce health disparities.
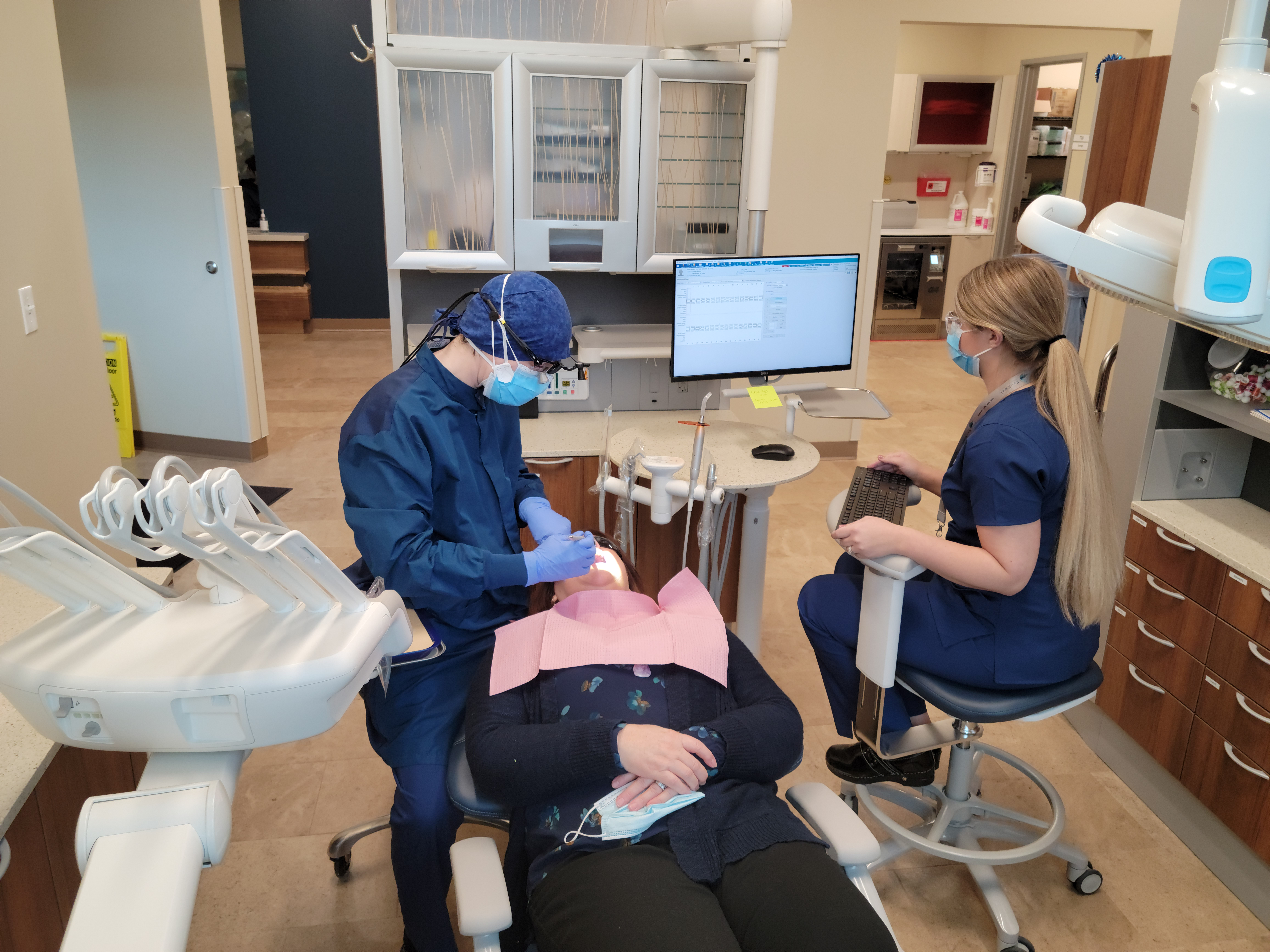
Holistic Care for All
Across the country, in Portland, Maine – the largest metro area in the nation’s most rural state – Greater Portland Health has been busier than ever during the Covid pandemic. A federally qualified health center, it provides high-quality healthcare to everyone regardless of their ability to pay. And three loans and two lines of credit from CEI ensured that the center not only stayed open but grew to meet demand for care.
The staff of 135 people working across 11 locations speak 12 different languages to accommodate a large immigrant and refugee population. A full suite of healthcare services includes medical, behavioral, and dental. Community members also receive financial counseling, peer support, and case management.
“Community health centers have worked to increase the number of services they provide when they see a need,” said Ann Tucker, CEO, Greater Portland Health. “We ask, ‘how can we, in our community, take care of the whole person?”
Mission-first financing coupled with community participation has been integral in Greater Portland Health’s ability annually serve over 10,000 people, half of whom are uninsured. CEI made its first loan to the center in 2013, the year Greater Portland Health transitioned from a city-supported pilot to an independent nonprofit.
“CEI was instrumental as one of our partners while we were getting our foundation under us,” said Tucker. “Without that investment in our health center, who’s to say we would be here today?”
At the time, the center was barely able to make payroll. No bank would consider a loan, but CEI worked closely with the leadership team to establish terms the center could meet. Subsequent financing from CEI allowed the center to invest in technologies and other improvements so that it can continue to provide healthcare to anyone who asks.

Filling Gaps in Health Center Financing, Deepening Mission Impact
Meeting healthcare needs for people in rural regions, and those who are uninsured and underinsured, is essential to the economic health of their communities. The overlapping missions of CDFIs and community health centers make them powerful allies in working together to connect people with the resources they need to reach their full potential. Their collaboration provides a collaborative path for catalytic philanthropic funders with place-based and community-centric missions. When CDFIs are able to fill financing gaps for community health centers, that impact is multiplied. Now the challenge is to build on successful community health models to reach the estimated 78 million residents living in Primary Care Health Professional Shortage Areas.



